The Great North Air Ambulance Service (GNAAS) has responded to 36 incidents in the Isle of Man since partnering with Manx Care last year.
The services began working together in March 2022 as part of a trial to develop a Helicopter Emergency Medical Service (HEMS), where seriously injured or unwell patients are transferred by helicopter from the Isle of Man directly to the UK for emergency medical treatment.
Prior to this partnership, GNAAS had already been established as a charity for nearly 20 years and has evolved from humble beginnings in May 2002 to being a world-class leader in pre-hospital care.

These are some of the key milestones the charity has achieved, which has led to them providing critical care to people in the Isle of Man.
In 2003 the charity introduced doctors to their team, which transformed the level of care offered to patients. This once revolutionary move has since been replicated across the country, and many air ambulance teams now consist of a pilot, doctor, and paramedic.
Since the introduction of doctor and paramedic critical care teams, the charity has recognised the importance of rigorous training and governance, which led to designing a bespoke training package emphasising the importance of multidisciplinary team working, proper decision making and robust governance procedures.
In 2007 the Pre-Hospital Emergency Anaesthesia (PHEA) course was launched which was the first of its kind in the UK. It is aimed at both doctors and paramedics and provides candidates with the knowledge and skills required to deliver pre-hospital anaesthesia.
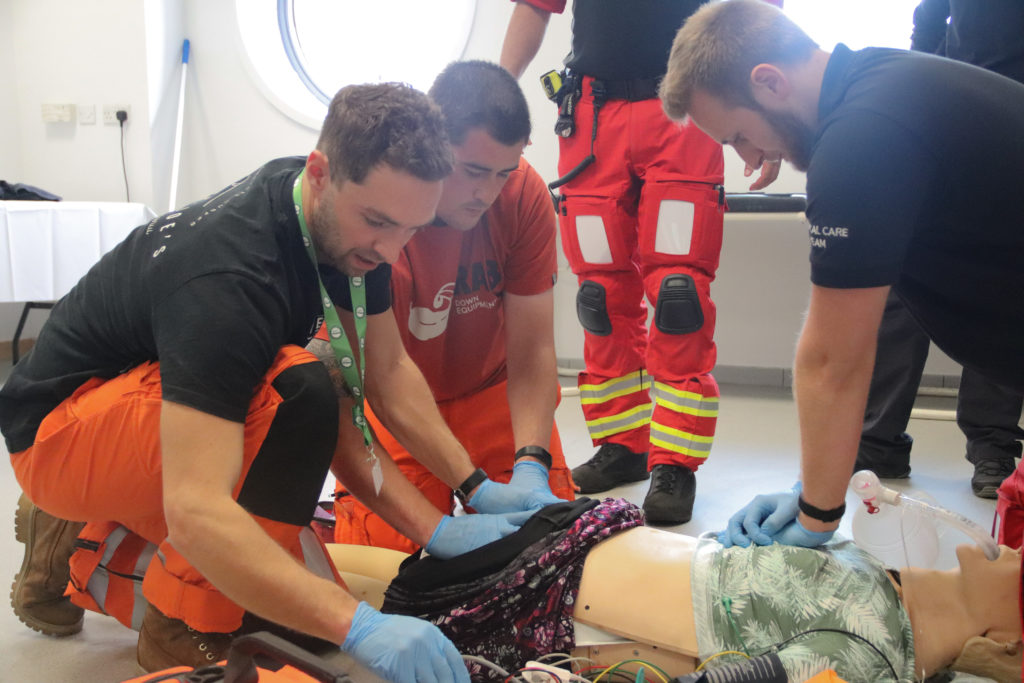
By 2014 two of the charity’s doctors took over the development and delivery of the course, leading to the formation of partnerships with County Durham and Darlington Fire and Rescue Service and Northumbria University, and was rebranded the ‘Pre-hospital Emergency Medicine Crew Course (PHEMCC) in 2015 and is now at the forefront of training in pre-hospital care internationally.
In 2015 blood was first carried on board GNAAS’ helicopters and rapid response vehicles, followed by the introduction of plasma the following year. The project was instigated by Dr Rachel Hawes, who received an OBE for her work, and the charity has now provided blood to more than 500 patients.

In 2017, GNAAS’ critical care team performed a successful thoracotomy when a man was stabbed and left for dead in County Durham in the North East of England. The surgery involves gaining access to the heart and lungs through a major incision in the chest. The man was literally brought back from the dead and the footage of it was the first time a successful pre-hospital thoracotomy had been recorded in the world. It has now become a vital training aid for pre-hospital teams.
In 2018, GNAAS became one of the first emergency services in the UK to utilise the GoodSAM app.
The app allows their team to see the scene through a bystander’s camera phone simply by sending them a text message and helps them make more informed decisions before deploying the aircraft to an incident.
The charity has also developed a software platform to manage, log and audit incidents they have attended. Previously they used a combination of paper and digital records, but now they have a fully digital database, and in 2019 they developed the system further by introducing a tablet version.

Last year GNAAS was given the highest possible rating of ‘Outstanding’ by the Care Quality Commission (CQC) following a recent inspection.
The CQC monitors, inspects and regulates services in every hospital, care home and healthcare provider, including air ambulance services, to make sure they meet fundamental standards of quality.
GNAAS received very positive feedback from the CQC’s head of hospital inspection who said they were extremely impressed by the level of care and support people received when using their service and there was a genuine culture of wanting to provide the best care for patients and a desire to improve services.
This sentiment is certainly echoed in one of the charity’s most recent achievements, which was becoming a 24/7 service in the North East of England at the start of 2023.
During the day the charity’s critical care team operate on an aircraft, however on the night-time they transfer to a rapid response vehicle. The car carries the same equipment as their aircraft, so the team can deliver blood, anaesthetic procedures and other advanced treatments, they just can’t airlift patients to hospital.

The charity hopes to offer the same level of service in Cumbria, UK, in the near future, and recently expanded from covering two nights to four nights in the county.
In addition to this, since March last year, GNAAS have been responding to incidents in the Isle of Man.
Prior to this arrangement, patients were transferred by fixed wing air ambulance but there was no access to a pre-hospital HEMS service which are able to provide the full spectrum of advanced critical care procedures, delivered by a doctor and critical care paramedic team.
Since the launch of the trial, GNAAS’ critical care teams, based in Penrith, Cumbria, and Teesside, North East, have been deployed 36 times.

They have carried out multiple interventions on the Island, which would not have been possible with a standard road paramedic crew, including putting patients in medically induced comas, administering blood transfusions, and carrying out surgical procedures.
To support the charity’s ongoing developments and build on their progress, they have recognised the need to increase their fundraising income and expand their fundraising reach.
This led to the recruitment of a fundraising lead for the Isle of Man in July, who is responsible for the fundraising events on the Island as well as creating awareness of the charity and the work that is carried out on the Island to support Manx residents.