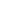“If I’m in the middle of a field or on a roadside, we have to plan and act there and then rather than rely on someone else to get involved.”
Kate Allen is a registrar in the busy emergency department at Sunderland Royal Hospital. For the last year, she’s also been training as an air ambulance doctor with the Great North Air Ambulance Service (GNAAS).
It’s fair to say it’s been something of a culture shock to go beyond the relative luxury of four walls into the pre-hospital frontier, where often the only equipment available is that which is carried on the clinician’s back.
“There’s lots of pressure – even more than I thought,” she said. “But I love it.”
Kate is halfway through a two-year training programme with GNAAS which will accredit her with a pre-hospital subspecialty. During the programme, Kate splits her time between work at the hospital and on the aircraft, which roughly equates to two days on each per week.
The biggest change Kate said she had noticed in herself was not necessarily from a clinical perspective, although she has picked up skills specific to the pre-hospital environment along the way, but was more in the way she handled the “human factors” of managing the scene of an incident.
“We are such a small team on scene and we are working in remote places,” she said. “In A&E, if I need help with an airway problem, I’ll ask an anaesthestist. But if I’m in the middle of a field or on a roadside, we have to plan and act there and then rather than rely on someone else to get involved.”
Kate’s progression as a pre-hospital clinician has had a knock-on effect on her hospital work as well.
“When I got the job, I worried a little that as I’m used to being part of a big team, it might be difficult adapting to working in a team of just two or three.
“But actually, in some respects, I now prefer having less people around in A&E. Instead, it’s all about having that well-drilled, well-briefed team with good communication that is so important with the air ambulance work.
“We are so spoilt in the UK in terms of having the availability of scans within 20 minutes of arrival at hospital. It means we don’t always need to rely on spotting problems as the machine will do that. You can’t rely on that out in the field – you have to be able to spot the symptoms of issues with a lung or spleen, for instance.”
Kate, originally from Bradford, joined GNAAS after applying through a national recruitment programme run by the Intercollegiate Board for Training in Pre-Hospital Emergency Medicine (IBTPHEM). The programme is aimed at creating a new generation of doctors who have focused on treating patients on the scene of an incident and in transit to hospital.
Last year, GNAAS clinicians published the first UK study which proves that a doctor and paramedic pre-hospital team improves survival from severe trauma. Lives are being saved and suffering eased on a regular basis as a result of the continued development of the air ambulance service and specifically the level of care on board. But this all depends on arming doctors like Kate with the skills and experience required to cope with the unique challenges posed by treating patients before they get to hospital.
Read more: How to become an air ambulance doctor
Kate applied through the national programme and nominated GNAAS as her preferred destination. After an interview and an assessment day with the charity, Kate was offered the post. But first she had to complete a month-long induction period which included the charity’s Pre-Hospital Emergency Anaesthesia (PHEA) course and the clinical and aviation modules of the Pre-Hospital Emergency Medicine Crew Course (PHEMCC), also run by the charity. She said this rigorous introduction, in which she learned from her future colleagues, has played a vital role in her adaptation to life on the aircraft.
She added: “I was on the course with clinicians from all over the country from all different organisations, but I was fortunate to be getting trained by the same people I ended up working with, so it was a good opportunity to get to know them and their way of working.
“I was also on the same course as GNAAS paramedic Steve Miles, for instance, and we worked closely together in that training environment. That experience of working as a team was beneficial when it came to us working together for real. We were able to hit the ground running.”