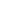In February this year, Kacper Krause, 13, of Appleby, drowned. He had been submerged in cold river water for around 25 minutes before being pulled out by brave staff from the town’s fire service.
In years gone by, the schoolboy would not have had a chance of survival. But thanks to specialist equipment and the expertise of healthcare staff, Kacper is making a strong recovery. Last week, just two months after the incident, he walked into the Great North Air Ambulance Service base at Langwathby to thank the charity’s critical care team.
The team on the aircraft that day was pilot Phil Lambert, paramedic Steve Miles and doctor Jeff Doran.
Following Kacper’s visit, Steve and Jeff recalled their involvement in an incident they said they would never forget.

What do you remember of the day?
Jeff – It was a Tuesday back in February, Steve and I were both on duty over at Durham Tees Valley Airport. Although the job came through to the North West Ambulance Service as a child drowning in Appleby, our Cumbrian aircraft, which would normally have been a slightly closer, was actually busy with another patient. So we saw the job come into the North West Ambulance Service and quite quickly we launched to that to try and provide support to the team that were already there. I think the flight took us about 15 minutes.
Steve – The weather was really good. A nice sunny day, lots of people out and about with it being so sunny.
Jeff – I remember it was late on in the afternoon, and I think it was about 5 o’clock in the evening. So the sun was still up but it was starting to set. I also remember as we were coming in we managed to land very close to the scene itself but there was a lot of people around.
Steve – I think that’s the first thing we kind of noticed, as we flew over the top that you could actually see all of the other emergency services already there and we managed to land really close, just slightly further along the riverbank.
Jeff – That was a big factor in it really because we could actually get to Kacper quite quickly, but I think when it came to us moving him from the riverbank into the helicopter it made things a lot easier because we were quite close to the actual site itself. So we both got on scene and as we arrived on scene, Kacper was already at the riverbank on the river side but he hadn’t been there very long.
Steve – We were told that he’d virtually just been rescued by the fire service as we landed.
Jeff – But they did have resuscitation started and he was receiving CPR and there was a first responder there from Appleby who was a GP I believe, and also Theo Weston, who works for GNAAS but was there as a rapid response doctor. Theo had intubated Kacper and so he had started the resuscitation process and so they were breathing for him using a breathing tube and controlling ventilation into the lungs with oxygen, and he was getting manual chest compressions at the time.
Steve – Those chest compressions were being handled mainly by the fire service who were doing a bit of a relay effort so that nobody got too tired and then almost immediately on our arrival we transferred that onto a mechanical chest compression device.
Jeff – You and I had actually spoken in the helicopter on the way over about the sort of things we might be expected to find and what we were going to do when we got there. I think that worked quite well because we’d already talked about the fact that it was likely to be very cold water and that this was almost certainly going to be a case of hypothermia. We knew we needed to treat that aggressively with quite a prolonged resuscitation attempt and we’d talked about the use of mechanical chest compression as part of that to stop things like fatigue and also to make it easier for us to look after Kacper. So we took the mechanical CPR device from the helicopter to Kacper and we started that very quickly.
Steve – Within a minute or so, the machine was on and running and then we decided to make some plans for an early move and you were able to ring ahead to the RVI.
Jeff – My role then was two-fold, one I spoke to Dion Arbid, who was the emergency department consultant at the Royal Victoria Infirmary. The reason being I wanted to give him a heads up that we were coming with a child who was severely hypothermic and in cardiac arrest and that we should consider getting the team over from the Freeman Hospital who could start what we call ECMO. This is where blood is taken out of the body, warmed and provided with oxygen before being delivered back to the body using a pump machine.
Read more: How ‘ECMO’ treatment saved drowned schoolboy
Jeff – ECMO is something that is available but there’s a lot of logistics that need to go into having that available for a patient because it’s quite complicated, so we thought about getting that done early. Dion was instrumental in getting that team across and having that facility available for Kacper. I’d left you managing the resuscitation and starting to think about the move, and I also went to speak to Kacper’s parents.
Steve – It was two things going at once; you were organising the onward care and speaking to Kacper’s parents so they knew what was happening, and at the same time you were doing that I was trying to expedite the move so that there was no delay so we could almost load straight into the helicopter once you’d finished the decision on the phone.
Jeff – While I was speaking to Kacper’s parents we had to move Kacper from the river edge into the helicopter which meant going down the side of the river, past where Kacper’s parents were stood, although there was a shield in place. As part of that as you were packaging him and getting ready to move Kacper, I spoke to his parents to explain what was happening and what needed to happen next and then I asked the police to try and create a way of moving Kacper as delicately as possible to the helicopter, as dignified as possible, and then we took him to the helicopter.

Steve – I remember being at the back of the helicopter, and I remember us having a little bit more chat about onward care and the different things we could do and I remember the flight time taking about 20 minutes which given where we were in Appleby, given the fact that it was such a nice day and the traffic on the road, it shortened that time measurably and made a massive difference in time. It would probably have taken well over an hour and a half, if not a bit longer from Appleby in that traffic condition, so being able to fly right across the top, straight to the RVI, with a waiting team really shortened the time to definitive care.
Jeff – This was definitely one of those circumstances where having access to a helicopter made a huge difference. One of the things that I remember was that we changed the battery on the mechanical CPR device just prior to going into the helicopter and the benefit of that was that from the minute we closed the doors on the helicopter to us arriving in the emergency department he had completely uninterrupted chest compressions and we know that that is one of the keys to survival in cardiac arrest where there is as little interruption as possible for the resuscitation efforts to maintain perfusion to the brain and the other vital organs. That for me was one of the keys – that he got to hospital quicker and he also had good quality resuscitation throughout that whole journey.
Steve – I think the whole of this case with Kacper just highlights the importance of that chain of survival in cardiac arrest. Right from the early recognition, the early bystander CPR, the early advanced care, to the hospital side of the care, it just shows that all those links in that chain are so important. What we were able to do was further bring that advanced care out in the pre-hospital environment, add to the care that he was already received on scene and then rapidly transfer him to that definitive care at the hospital.
Jeff – As we got to the RVI because we’d been able to pre-alert them and warn them about what was happening on scene and what we felt needed to happen thereafter, the arrangements had already been made and some of the Freeman team were already actually waiting for us as we arrived in the emergency department. They had a full critical care team there including pediatricians and intensive care doctors, as well as the emergency department team led by Dion, and he got good continuity of care from the moment Steve and I handed him over he went onto their mechanical cpr device and there was a really good handover period. And then the Freeman team were able to come as well in the next few minutes to begin the ECMO therapy.
What was it like meeting the family again?
Steve – Amazing. I think this is what the job’s all about. This is what we aim to achieve with every patient. You want a good outcome and to meet somebody like this. Last time I saw Kacper he was being resuscitated, he had no signs of life, and to meet him, talk to him, see him walking, is brilliant, absolutely fantastic.
Jeff – I think we try and make a difference in every case that we go to. It’s nice when we have these really good positive outcomes – to be able to go away and reflect after the incident and then come back and actually enjoy what is a much more joyful experience. It’s one of the cases that I’ll remember throughout my career.
GNAAS is reliant on donations to survive. To donate today, please click here.